Understanding, Symptoms and Diagnosis
What is an autoimmune disease?
What is the difference between an autoimmune disease and an immune disease?
Unfortunately, the foundation must focus on autoimmune diseases 🎯 to target and support researchers.
👉 Immune disease is a broad term that encompasses all disorders of the immune system.
This includes:
• when the immune system is overactive
• when it is misdirected
• when it is insufficient
📌 In summary: All autoimmune diseases are immune diseases, but not all immune diseases are autoimmune. ⸻
⚠️ Autoimmune Disease (subcategory)
👉 An autoimmune disease is a specific immune disease where:
• the immune system mistakenly attacks the body's own cells
• the body no longer distinguishes between "self" and "non-self"
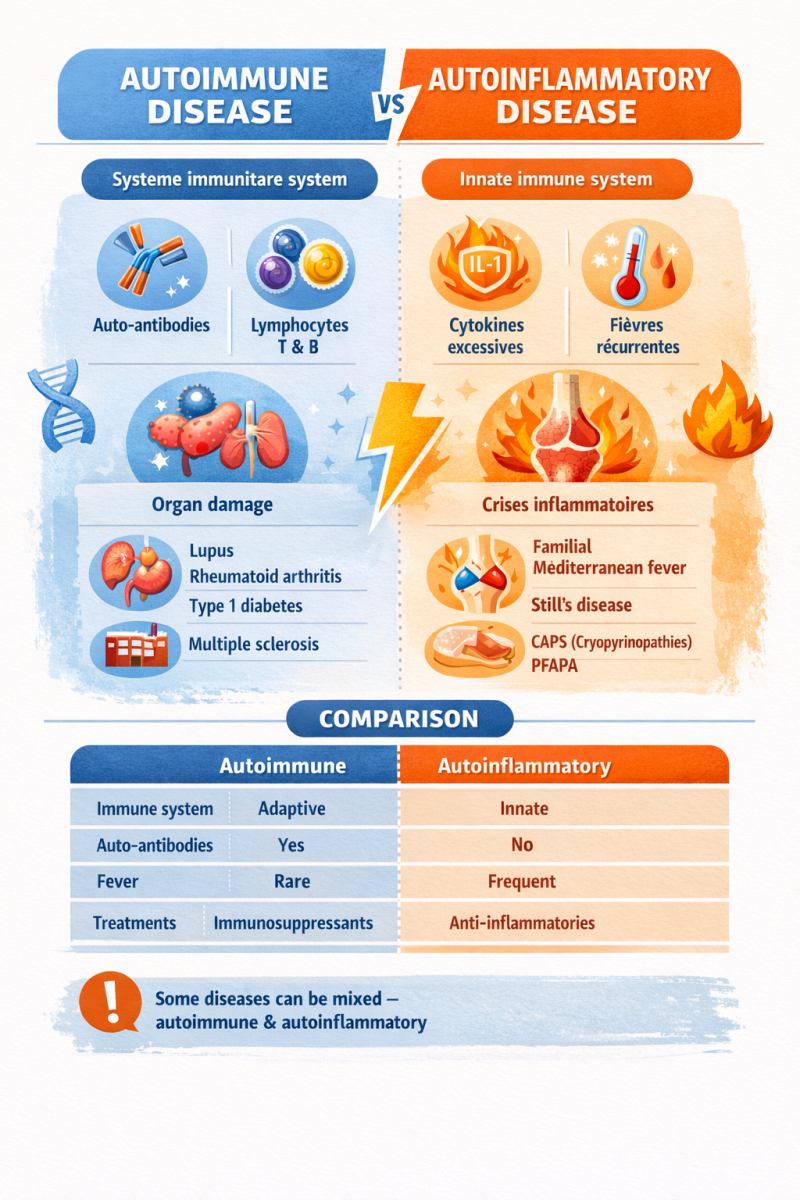
Difference between a disease and a syndrome
What is the difference between a disease and a syndrome?
🦠 Disease
A disease is a well-defined medical condition.
Characteristics:
• An identified or strongly suspected cause (autoimmune, genetic, infectious, etc.)
• Known or increasingly well-understood biological mechanisms
• Clear diagnostic criteria (tests, labs, imaging)
• A relatively predictable course and standardized treatments
Examples:
• Type 1 diabetes
• Rheumatoid arthritis
• Multiple sclerosis
In short: we know what it is, why it happens, and how to diagnose it.
⸻
🧩 Syndrome
A syndrome is a group of signs and symptoms that tend to occur together, without a single clearly identified cause.
Characteristics:
• A recurring pattern of symptoms
• Mechanisms that are partially understood or still unknown
• Diagnosis is mainly clinical (based on symptoms)
• May later be reclassified as a disease as scientific knowledge advances
Examples:
• Sjögren’s syndrome
• Irritable bowel syndrome
• Chronic fatigue syndrome
In short: we describe what is happening, but not always why.
💡 Important takeaway
A syndrome is not less real or less serious than a disease.
It is often a stage in scientific understanding.
👉 Many conditions called syndromes today will likely be recognized as diseases in the future as research progresses.
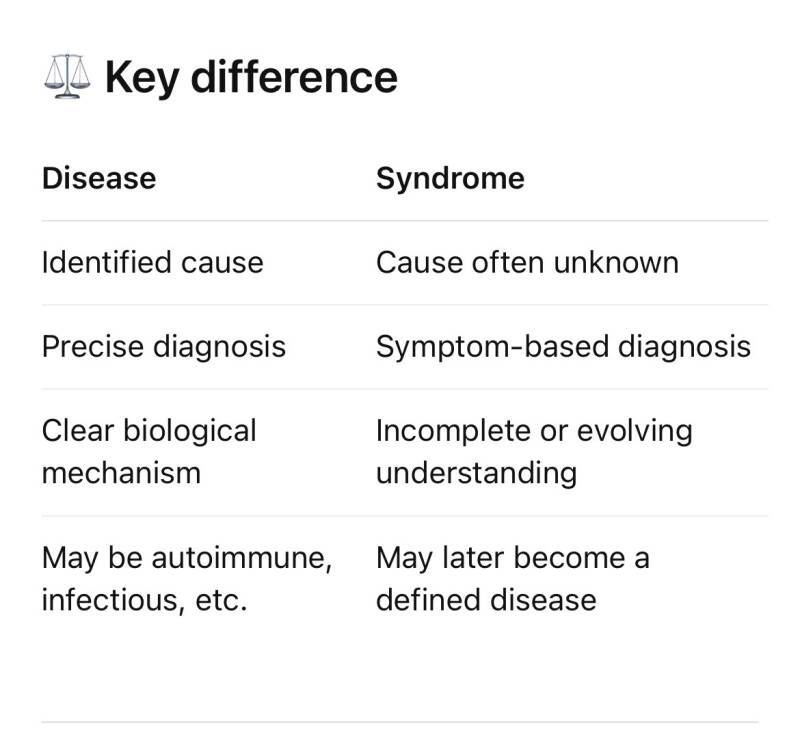
Common symptoms
An autoimmune disease is a condition in which the immune system mistakenly attacks the body's own cells, identifying them as enemies. This can lead to chronic inflammation, pain, and organ damage.
Common Symptoms (Vary depending on the disease)
Intense and persistent fatigue
Joint or muscle pain
Inflammation
Unexplained fever
Digestive problems
Neurological problems
Skin rashes
Hair loss
Possible Causes
The exact causes are still poorly understood, but the following are suspected:
Genetic factors
Infections (triggering)
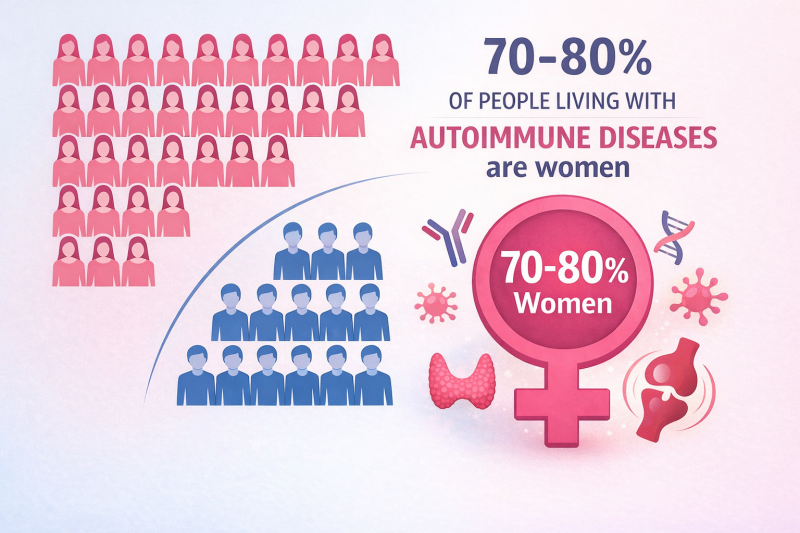
Hormones (women are more affected because they have two X chromosomes, men only one). This explains why there are twice as many cases in women.
Environmental factors (stress, toxins, pollution)
Treatments
In Canada, only the symptoms are treated according to their severity and impact. There are no cures approved for general public use.
Do you know why WOMEN are more affected (70-80%)
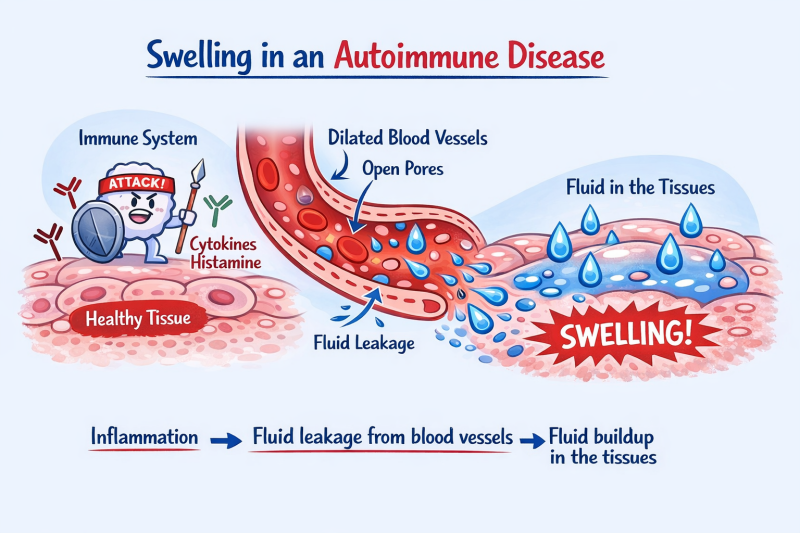
Why is SWELLING so present in #autoimmune disease?
Why is #SWELLING so present in #autoimmune disease?
Normally, swelling is a temporary and essential protective response of the body. It signals an immune response to isolate an injured or infected area, providing white blood cells and nutrients for healing.
Here's how swelling protects the body:
It results from the influx of blood and liquids, providing nutrients and immune cells to repair tissues and eliminate pathogens (bacteria, viruses).
Forced immobilization: By increasing pressure and pain, swelling limits the mobility of the affected area, thus avoiding aggravating the injury.
Isolation: The accumulated liquid helps isolate the injured area to prevent the spread of an infection.
____
Swelling in AUTOIMMUNE DISEASES results from an erroneous immune reaction where the body attacks its own tissues (skin, intestine, muscles, rash, etc.)
Although beneficial at first (acute inflammation), an inflammation that persists (chronic) is no longer protective and can cause tissue damage.
The immune system sends white blood cells and hormones that dilate blood vessels, causing swelling.
The immune system is in permanent “attack” mode.
Normally, the vessels keep the liquid inside.
In #autoimmune inflammation, there is a leak of liquid from the vessels
• the "pores" of the vessels open
• the plasma escapes to the tissues
Liquid accumulates → swelling
#Autoantibodies (bad antibodies) attach to tissues
This amplifies the inflammation
Attracts even more immune cells to try to fight
Result: even more swelling
"We must work on the source of antibodies, not only to reduce symptoms! Let's encourage #Autoimmune research"
How to detect an autoimmune disease and the diagnostic odyssey
Studies (primarily conducted outside Canada but applicable to the clinical context) indicate that the average diagnostic delay is four years.
Difficulty accessing a doctor, lack of knowledge, limited access to specific tests, often common symptoms such as fatigue and muscle pain, and a shortage of medical specialists all contribute to the challenges of accessing care and the diagnostic odyssey.
There is no single test to "detect an autoimmune disease." Diagnosis relies on a combination of tests, along with symptoms and a clinical examination.
🧪 1. Basic blood tests = looking for signs of inflammation
👉 Often the first tests ordered
• CRP (C-reactive protein) → active inflammation
• ESR (erythrocyte sedimentation rate) → chronic inflammation
• Complete blood count (CBC)
• anemia
• abnormal white blood cells
• high or low platelets
📌 These tests don't specify "which" disease, but they show that something is wrong.
🧬 2. General immunological tests (autoimmunity)
• ANA (antinuclear antibodies)
🎯 3. Specific Autoantibodies (the most important)
These tests point to a specific disease
🔹 Rheumatological Diseases
• Anti-dsDNA → lupus
• Anti-Sm → lupus (very specific)
• Anti-SSA/SSB → Sjögren's syndrome, lupus
• Anti-RNP → mixed disease
• Rheumatoid Factor (RF) → rheumatoid arthritis
• Anti-CCP → polyarthritis (very specific)
• HLA-B27 (SPA) → Spondyloarthritis
🔹 Endocrine Diseases
• Anti-TPO: Hashimoto's thyroiditis
🔹 Autoimmune Neurological Diseases
• Anti-GAD → SPS, type 1 diabetes
• Anti-NMDA, LGI1, CASPR2 → autoimmune encephalitis
• Anti-AQP4 / MOG → neuromyelitis optica
🔹 Digestive Diseases
• Anti-transglutaminase (IgA) → celiac disease
• pANCA / ASCA → IBD (Crohn's disease / colitis)
🔹 Dermatological Diseases
• Anti-BP180 / BP230 → bullous pemphigoid
• Anti-desmoglein → pemphigus
🧫 4. Complement
(very important and often overlooked)
Indicates abnormal activation of the immune system
• C3, C4
• CH50
My anxiety and stress? Is it me or my illness?
Do you know about GABA?
This post will be one of my most personal because I live with this every day. I live with Stiff Person Syndrome (SPS).
My bad antibody is called AntiGAD65 and it attacks my GABA.
So, my first subject of study was GABA.
GABA is a neurotransmitter that activates my inhibitory system to calm my excitatory system.
So I no longer have any "Zen" 🤣
I have stiff muscles, I'm often anxious, I have inflammation, and I even broke a tooth from clenching my jaw too hard! So, you now understand a little about Stiff Person Syndrome.
But what about other autoimmune diseases?
Glutamate is the neurotransmitter that activates the neurological excitatory system.
n autoimmune diseases, the balance between glutamate and GABA is often disrupted, contributing to neuroinflammation and neuronal degeneration.
By 2026, modulating the GABAergic and glutamatergic systems is a major therapeutic avenue for slowing the progression of autoimmune diseases and protecting the nervous system against neuroinflammation.
So, the next time you ask yourself, "Is it me or my illness?" know that your GABA imbalance can play tricks on you, and you'll feel better tomorrow 🫶

